Today, I receive a lot of misplaced pity, another (preventable this time) death occurs in the hospital, and the specialist urologist surgeon arrives while i spend much of the day in outpatients.
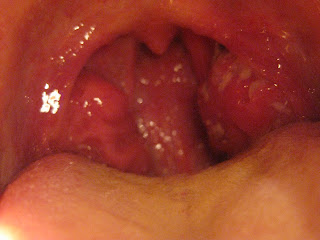
The continual pity that seems to be showered down upon me, because I am feeling (and probably looking) very ill must be because I am a mzungu, either as they want to care for their guests (more likely), or they think it must be hard for me to be ill, as mzungu have no idea about suffering (relatively true). Though I am unable to swallow any food, I can still Speak and intend to keep turning up for things. After all the excitement, planning and cost that went into this, I do not plan on spending it in bed. I have been looking forward to this elective since before I started medical school, and plan to make the most of it. Please see my tonsils, below, for their patchy beauty.
My painful tonsils with all their annoying patches on them. I suppose its better than getting HIV.
Chief came around last night, for what is becoming his regular chat, peered into my mouth at my spotty white tonsils (image above) and persuaded me to go on amoxicillin. I do not usually take medications, and I am sure that this will go on its own, but I really do want to get better, and he is very experienced so I will do as he says. I know in the UK that amoxicillin is rarely used for these sorts of infections, because of the risk of it being glandular fever. Epstein–Barr virus and amoxicillin can react together and create a rash across the entire body. I tell Chief this but he tells me not to be silly. In some ways, I hope that I do get this diffuse rash all over my body, it would be exciting and kinda prove me right. But in many more ways I just want to feel better.
Today, for ease, I spent most of my time (after a wander through the wards) in outpatients, as here I could sit down. The specialist urologist arrived today, and the OPD department is extraordinarily busy, as word has been spread throughout the region about the specialist's arrival. Unfortunately, most patients have come with non-urology causes, hoping to see the specialist anyway. The assumption here seems to be that specialists are better doctors, so should be the ones to see your problem, whether it is in their field of knowledge or not. Tim the Tanzanian medical student is working in OPD again in one room with a doctor in the other. There is only really one room for a doctor to consult in, so our consultations are taken in a waiting and observation room, where patients wait to be seen, and nurses take temperatures and other observations. Last time I was with Tim I enjoyed the challenge of communal decision making (read: neither of us knowing what to do), and feel I would be more helpful with him than with a qualified doctor (Dr BT).
We see numerous patients with a rainbow of complaints, only three of whom we refer to the urologist. A lady with probable renal stones, and two possible congenital malformations. These are both boys who have repetitively had urinary tract infections, again and again, and various other problems with urination, such as leakage of urine accidentally. These are the sort of people that hopefully the urologist can help. A huge issue here is the small number of diagnostic tests available. Huge amounts rely on the history, which as I will talk about later, cannot always be relied upon. It is amazing how much is available in the NHS hospitals, with specialists just down the corridor to carry out advanced tests just when they are asked to help.
Tim and I have developed a good teamwork technique. As he talks Swahili he talks to the patient or translating relative, relaying information back to me, which I write in the notes. I suggest further questions (such as, is there blood or mucus in the diarrhoea?) depending on what they have said, which he then translates and asks for me. I have been taught much more thorough history taking skills, and have had much more in-depth teaching about ideas for investigations to be carried out for certain presentations, while Tim has a much better prescribing knowledge, not just of which drugs are available but of which doses are needed, and the length of course required for certain diseases. With his linguistic and drug knowledge, and all of the history taking teaching that has been drummed into me we make a fine team. Jack Sprat and all of that. At least I hope we make a good team, at least no-one has complained yet, and I enjoy being made to feel useful!
Among the afore-mentioned-rainbow of patients seen today was a severely constipated man, who on further questioning revealed that he drank 8L of local brew alcohol a day (home brewed is usually quite weak, Tim tells me), therefore not eating as he wasn't hungry. He refused our reasons for constipation and didn't want to accept our lifestyle advice. He got a de-worming pill (as we have to give every one medications) but I don't think they would have survived all that booze...
Among the afore-mentioned-rainbow of patients seen today was a severely constipated man, who on further questioning revealed that he drank 8L of local brew alcohol a day (home brewed is usually quite weak, Tim tells me), therefore not eating as he wasn't hungry. He refused our reasons for constipation and didn't want to accept our lifestyle advice. He got a de-worming pill (as we have to give every one medications) but I don't think they would have survived all that booze...
There were a couple of the typical fussy mums, complaining that their Children had runny noses, as the child ran around the consulting room in full health. I am sure GPs in the UK see many similar issues to this. I (would like to think that I) would have been more sympathetic if not feeling so poorly myself. Good thing I was not doing the talking!
We also saw a number of gynaecological patients in the clinic today. One was particularly confusing, with symptoms that changed back and forth as the conversation progressed. She may have had endometriosis, PID or fiboids. Or all three. She seemed to have every single gynaecological complaint you could have thought of. Tim comes to the rescue, explaining that some patients present friends symptoms as their own to avoid numerous consultation changes, hoping to get medication for their disease and their friends problems. How complicated! Tim performs a vaginal examination (much harder than it seems, given that there is not actually a couch in the room, or a lock and only a curtain behind us into the next room rather than a door) and reports a strange smelling discharge. We hedge our bets on PID and offer a follow up to see if it improves.
Today a woman had a still born baby at term (after 9 months). This was pretty upsetting. Not just because a baby was lost, but because there is a chance it could have been prevented. The mother was admitted yesterday with headache and visual disturbance so bad she could not see the keys on her phone to call anyone. On her admission the nurse took the usual obs including a blood pressure of 100/70. Nothing much was done as there were other priorities for a while, and she didn't seem a priority. The foetal heart could still be heard. Later, the woman had a further blood pressure done, which read at 220/160. This is very very high. In the subsequent kerfuffel where nurses tried to find one of the elusive doctors, the woman started bleeding heavily (perhaps a ruptured placenta due to the high blood pressure) and the baby was still born. It seems if is common for nurses to invent obs data if they feel they do not have the time or inclination to actually carry out the tests. The fact Some of the BP machines are broken does not help. Its possible this loss would still have happened even if the BP had been taken the first time, but its possible she could have been observed more closely and prepared for Cesarean. Really, I thought it was inexcusable. I was very impressed with Chief's altitude towards this though. He was very calm, talking about the importune of taking care with each measurement, and he didn't even suggest anyone was to blame. A fantastic leader. On of my (many) faults is that I do not really suffer fools gladly, and if I had been in his position I would have been very annoyed at this nurse for being involved in this babies death. Things do seem different in Tanzania, though, and this event was never mentioned again. In the UK I am sure there would have been some form of inquest.
In the afternoon, I headed down to help the Urologist carry out his clinic. Seeing all the potential patients for surgeries over the next week, there are dozens of people who want surgery. Dr Bike is outside, and tells Me I Should rest at home. Considerate but I say I would prefer to do something. He tells me to Come back in two hours, at 5 PM. On this return, I am told that I am far too late to help as many patients have already been seen. I am Suspicious of Dr Bike for his motives of forcing me to rest, but do not bring it up. I am sure it was meant to be in my best interests.
The male ward, patients admitted for operations from the urologist. The drip stand on the right of the picture is a plank of wood with a nail at the top.
Resting at home, the urologist returns and we chat, me diplomatically avoiding the fact that while I don't know what I want to specialise in, urology is one of the few on My definite no list. To reward my diplomacy, I am invited to assist in a list of turp operations. Perhaps tomorrow I will be too sick to help...




In fairness, if Chief was a bit more hard-line, that mightn't have happened as the nurse would've known she'd be in serious trouble for not checking the BP initially. I'm not sure if the forgive+forget everything attitude is the best way to run a hospital.
ReplyDeleteEnjoying the blogs!