Hi,
I am feeling mostly better now, which is great! Wasn't as great towards the start of the week, so I didn't go into the hospital much, but I did go into a teaching session with a consultant and a couple of other medical students, where we practice ENT examinations on each other. I also hear from a friend about some shocking sexism she was exposed to, from a surgeon who is a well known misogynist...
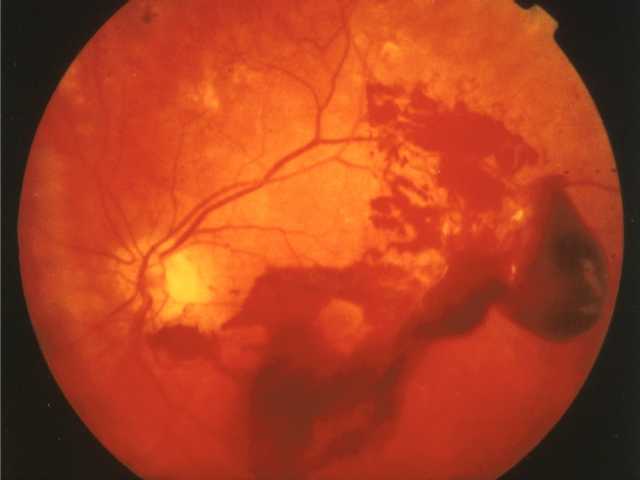
Most of our teaching comes from talking to patients, and trying out examinations or procedures on them. See the BBC 'Junior Doctors - Your Life in Their Hands' to see what I mean (though I don't really think that much of that that programme, many of them just seem so... unlike-able...). Hence why a few weeks ago I was practising ophthalmoscopy on patients under the directions of a consultant. The ENT consultants have decided that, rather than trying out all these ear, nose, throat examinations on patients - it would be a lot better for us to try them on each other, learning how not to hurt people by being hurt / hurting one another. A good idea, and its great to be taught examinations and so on as you do them, rather than read up on them and pretend you know what you are doing (as I have done before for an ABG).
The problem with being taught on one another is that if there is something... gross.. in the examination it is a lot more personal. When you are with patients it is all par for the course and expected, but with each other it is a little bit stranger. I was doing this with 2 medical students, and the male one (slightly low on tact) was examining the females ears, when he remarked 'wow I can hardly see anything, these are full of earwax'. Clearly something that is very normal, ears produce wax, and some ears produce more than others... Not something you usually want to hear about your class mate though, and the girl was clearly a bit hurt by this. When I was later examining his nose, it had this giant bogie sitting it it , wobbling around - again, normal for a patient, the nose makes these things, but strange to be peering at a class mates! (at least it wasn't as bad as this one!). With my messed up throat after the tonsil operation, we all had something on the examination to see, just strange to see it on a fellow medical students. Perhaps this is why doctors are not meant to treat their friends or family!
Later in the week, on of my female friends was complaining about how she had been treated when she went into surgery (perhaps on a different rotation, perhaps not - who knows!). The consultant is a well known misogynist, and has previously voiced his opinion that he feels that women are wasting their time in medicine, and would be much more suited to being at home and looking after children. This is clearly quite a... contentious... opinion... Anyway, this consultant was asking the medical student questions, some of which she didn't know the answer to. Pretty standard, but this consultant was clearly not impressed. He asked some harder very obscure questions that she clearly wouldn't have a clue about, then told her she was wasting her time at medical school, because she was too stupid, and may as well leave. He then went on to say she would be a rubbish doctor, and he would write to her parents to tell them that they were wasting their money on her course fees... How rude! And misguided! Who pays their course fees up front now (top up fees), and everyone relies on student loan... There was no reason of him to say things like that other than to be rude and offend her. It was probably because she was a girl, as he doesn't speak like this with any males... It is a shame that the world of medicine is such a hierarchical place. I would love to think that if that happened to me, I would stick up for myself, but really it is hard to do. You cannot afford offending some consultant who signs off your clinical books, then acts as an examiner in clinical examinations later in the year. I would also like to think that I would stand up for someone if I was there, but I don't really know what I would do - such a risk, but would you be able to keep quiet?